Understanding Varicose Veins: A Comprehensive Patient Guide

Varicose veins affect millions of Americans, yet many people who develop these enlarged, twisted veins don't fully understand what causes them, why they occur, or what can be done to treat them effectively. This comprehensive guide provides essential information about varicose veins, helping patients understand their condition, recognize symptoms, identify risk factors, and make informed decisions about treatment options that can improve both their appearance and quality of life.
Understanding varicose veins begins with recognizing that these visible, often uncomfortable vessels are not simply a cosmetic concern but rather a manifestation of underlying venous disease that can progress over time if left untreated. While varicose veins may start as a minor aesthetic issue, they can develop into more serious problems that affect mobility, comfort, and overall health if not properly addressed by experienced vein specialists.
BASS Vein Center's decades of experience treating patients with varicose veins have provided deep insights into how these conditions develop, progress, and respond to various treatment approaches. This expertise, combined with a commitment to patient education, helps individuals understand their condition and make informed decisions about their vein health that can lead to improved outcomes and better quality of life.
What Are Varicose Veins?
Varicose veins are enlarged, twisted, and often bulging veins that typically appear on the legs and feet, though they can occur in other areas of the body as well. These veins develop when the normal flow of blood through the venous system is disrupted, causing blood to pool and veins to become enlarged and distorted. Understanding the basic anatomy and function of the venous system helps explain how and why varicose veins develop.
The venous system is responsible for returning blood from the body's tissues back to the heart, working against gravity when we're standing or sitting upright. This challenging task is accomplished through a series of one-way valves within the veins that prevent blood from flowing backward due to gravitational forces. When these valves function properly, blood moves efficiently toward the heart with each muscle contraction and valve closure.
Varicose veins develop when these crucial valves become damaged or weakened, allowing blood to flow backward and pool in the affected veins. This backward flow, called venous reflux, causes increased pressure within the veins, leading to their characteristic enlargement, twisting, and bulging appearance. The affected veins may become visible through the skin as dark blue, purple, or greenish lines that can range from small, thread-like vessels to large, rope-like structures.
The appearance of varicose veins can vary significantly from person to person, depending on factors such as the size of the affected veins, the depth beneath the skin surface, and individual skin characteristics. Some varicose veins appear as small, web-like clusters near the skin surface, while others may bulge prominently and feel firm or tender to the touch. The color can range from blue or purple to dark green, and the texture may be smooth or have a twisted, rope-like appearance.
It's important to understand that varicose veins are not simply enlarged normal veins, but rather diseased vessels that are no longer functioning properly. This distinction is crucial because it explains why varicose veins often cause symptoms beyond their visible appearance and why they may require medical treatment rather than simply cosmetic intervention.
The Underlying Causes of Varicose Veins
Understanding what causes varicose veins helps patients recognize their risk factors and take appropriate steps to prevent or minimize their development. While some causes are beyond our control, others can be influenced through lifestyle choices and preventive measures.
Genetic predisposition plays a significant role in varicose vein development, with family history being one of the strongest predictors of who will develop these conditions. If one or both parents have varicose veins, their children have a significantly increased likelihood of developing them as well. This genetic component affects the strength and structure of vein walls and valves, making some individuals more susceptible to venous insufficiency.
Age-related changes in the venous system contribute to varicose vein development as the natural aging process affects the elasticity and strength of vein walls and valves. Over time, the constant work of pumping blood against gravity takes its toll on the venous system, leading to gradual weakening of valve function and increased risk of venous reflux.
Hormonal influences, particularly those related to female reproductive hormones, significantly impact varicose vein development. Estrogen and progesterone can affect vein wall strength and valve function, which explains why women are more likely to develop varicose veins than men and why these conditions often worsen during pregnancy, menstruation, or hormone replacement therapy.
Pregnancy creates multiple risk factors for varicose vein development, including increased blood volume, hormonal changes, and physical pressure from the growing uterus on the major veins that return blood from the legs. Many women first notice varicose veins during pregnancy, and these may worsen with subsequent pregnancies.
Occupational factors that involve prolonged standing or sitting can contribute to varicose vein development by increasing venous pressure and reducing the muscle pump action that helps move blood through the veins. Jobs that require long periods in static positions, such as teaching, nursing, retail work, or desk jobs, may increase the risk of developing varicose veins.
Lifestyle factors, including obesity, lack of exercise, and poor dietary habits, can contribute to varicose vein development by affecting circulation, increasing venous pressure, and reducing the efficiency of the muscle pump mechanism that helps move blood through the veins.
Recognizing the Symptoms of Varicose Veins
Varicose veins can cause a wide range of symptoms that extend far beyond their visible appearance, and understanding these symptoms helps patients recognize when they should seek medical evaluation and treatment. Many people are surprised to learn that varicose veins can cause significant discomfort and functional limitations.
Leg heaviness and fatigue are among the most common symptoms associated with varicose veins, often described as a feeling that the legs are weighted down or difficult to move, particularly after periods of standing or at the end of the day. This heaviness typically improves with leg elevation or walking and may be one of the earliest signs of developing venous insufficiency.
Aching and pain in the legs can range from mild discomfort to significant pain that interferes with daily activities. This pain is typically described as a dull, throbbing sensation that worsens with prolonged standing or sitting and improves with movement or leg elevation. The pain may be localized to areas where varicose veins are visible or may affect the entire leg.
Swelling, particularly around the ankles and lower legs, often develops as varicose veins progress and venous pressure increases. This swelling typically worsens throughout the day and may be accompanied by a feeling of tightness in the legs or difficulty fitting into shoes that were comfortable in the morning.
Burning or throbbing sensations along the course of varicose veins can be particularly bothersome and may interfere with sleep or daily activities. These sensations may be constant or intermittent and often worsen with prolonged standing or during warm weather.
Itching around varicose veins is a common symptom that can be quite bothersome and may lead to scratching that can damage the skin and increase the risk of complications. This itching is often related to poor circulation and skin changes that occur as varicose veins progress.
Muscle cramps, particularly at night, can be associated with varicose veins and may significantly impact sleep quality. These cramps often occur in the calf muscles and may be related to poor circulation and fluid accumulation in the legs.
Restless leg syndrome, characterized by an irresistible urge to move the legs, particularly when resting or trying to sleep, can be associated with varicose veins and venous insufficiency. This condition can significantly impact sleep quality and overall quality of life.
Risk Factors and Prevention Strategies
Understanding the risk factors for varicose vein development helps individuals take proactive steps to prevent or minimize their occurrence. While some risk factors cannot be changed, many can be influenced through lifestyle modifications and preventive measures.
Non-modifiable risk factors include genetics, age, and gender, which cannot be changed but help identify individuals who should be particularly vigilant about prevention and early detection. Women are more likely to develop varicose veins than men, and the risk increases with age for both genders.
Modifiable risk factors offer opportunities for prevention and include weight management, exercise habits, occupational factors, and lifestyle choices. Understanding these factors empowers individuals to take control of their vein health and reduce their risk of developing problematic varicose veins.
Weight management plays a crucial role in varicose vein prevention, as excess weight increases pressure on the leg veins and can impair circulation. Maintaining a healthy weight through proper diet and exercise helps reduce the strain on the venous system and decreases the risk of developing varicose veins.
Regular exercise, particularly activities that engage the calf muscles such as walking, swimming, or cycling, helps improve circulation and strengthen the muscle pump mechanism that assists venous return. Exercise also helps with weight management and overall cardiovascular health, providing multiple benefits for vein health.
Occupational modifications can help reduce the risk of varicose veins for individuals whose jobs require prolonged standing or sitting. Taking regular breaks to move around, using compression stockings, and elevating the legs when possible can help reduce venous pressure and improve circulation.
Dietary considerations that support vein health include maintaining adequate hydration, consuming foods rich in antioxidants and anti-inflammatory compounds, and limiting sodium intake to reduce fluid retention. A diet rich in fruits, vegetables, and whole grains provides nutrients that support vascular health.
Clothing choices can impact vein health, with tight-fitting garments around the waist, groin, or legs potentially restricting circulation and increasing venous pressure. Choosing comfortable, well-fitting clothing and avoiding high heels for extended periods can help support healthy circulation.
When to Seek Medical Evaluation
Knowing when to seek medical evaluation for varicose veins is important for preventing progression and complications while ensuring that treatment is initiated at the optimal time for the best outcomes. Many people delay seeking treatment, thinking that varicose veins are purely cosmetic, but early intervention can prevent more serious problems.
Visible varicose veins, even if they're not causing significant symptoms, warrant medical evaluation to assess the underlying venous function and determine if treatment is recommended. Early evaluation allows for monitoring of the condition and intervention before symptoms become severe or complications develop.
Symptomatic varicose veins that cause leg heaviness, aching, swelling, or other discomfort should be evaluated promptly, as these symptoms indicate that the varicose veins are affecting circulation and quality of life. Treatment of symptomatic varicose veins can provide significant relief and prevent progression.
Progressive symptoms that worsen over time or interfere with daily activities indicate the need for medical evaluation and likely treatment. Varicose veins tend to worsen over time if left untreated, so progressive symptoms suggest that intervention may be beneficial.
Skin changes around varicose veins, including discoloration, thickening, or the development of sores or ulcers, require immediate medical attention as these changes indicate advanced venous disease that needs prompt treatment to prevent serious complications.
Bleeding from varicose veins, while uncommon, requires immediate medical attention as it can be difficult to control and may indicate significant venous pressure or skin breakdown. Any bleeding from varicose veins should be evaluated promptly by a vein specialist.
Family history of serious venous complications, such as blood clots or venous ulcers, may warrant earlier evaluation and more aggressive monitoring, even if current symptoms are mild. Understanding family history helps guide appropriate screening and prevention strategies.
Understanding Treatment Options
Modern treatment options for varicose veins offer excellent outcomes with minimal discomfort and downtime, making it easier than ever for patients to address their vein problems effectively. Understanding these options helps patients make informed decisions about their care.
Conservative treatment approaches, including compression stockings, lifestyle modifications, and symptom management, may be appropriate for some patients, particularly those with mild symptoms or who are not candidates for more invasive procedures. These approaches can help manage symptoms and may slow the progression of the condition.
Minimally invasive procedures have revolutionized varicose vein treatment, offering excellent outcomes with minimal discomfort and rapid recovery. These procedures, including endovenous ablation, sclerotherapy, and ambulatory phlebectomy, can effectively treat varicose veins while allowing patients to return to normal activities quickly.
Endovenous ablation procedures use energy-based techniques to close problematic veins from the inside, eliminating the source of venous reflux and allowing blood to reroute through healthier vessels. These procedures are highly effective and can be performed in an office setting with local anesthesia.
Sclerotherapy involves injecting a solution into problematic veins that causes them to close and eventually be absorbed by the body. This technique is particularly effective for smaller varicose veins and spider veins and can often be combined with other treatments for comprehensive results.
Ambulatory phlebectomy is a surgical technique that allows for the removal of large, bulging varicose veins through tiny incisions that typically heal with minimal scarring. This procedure can provide immediate improvement in the appearance of prominent varicose veins.
Combination treatment approaches often provide the best outcomes for patients with complex varicose vein problems, using different techniques to address different aspects of the condition. Experienced vein specialists can develop comprehensive treatment plans that optimize outcomes while minimizing treatment burden.
The Importance of Professional Evaluation
Professional evaluation by experienced vein specialists is essential for accurate diagnosis, appropriate treatment planning, and optimal outcomes. Understanding what to expect during a professional evaluation helps patients prepare for their consultation and make the most of their appointment.
Comprehensive history taking involves a detailed discussion of symptoms, family history, medical conditions, medications, and lifestyle factors that may contribute to varicose vein development. This information helps guide the physical examination and diagnostic testing while identifying factors that may affect treatment planning.
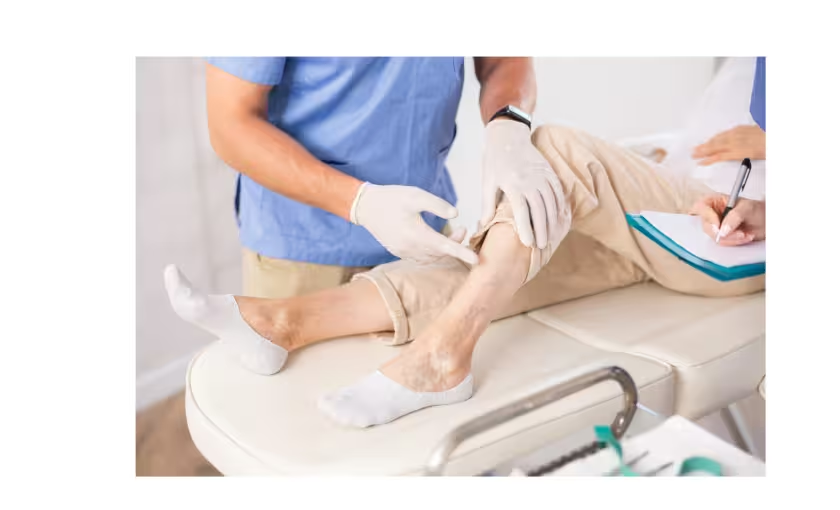
Physical examination includes visual inspection of the legs, palpation of varicose veins, and assessment of skin changes or other signs of venous disease. The examination is typically performed with the patient standing to allow for proper evaluation of vein filling and valve function.
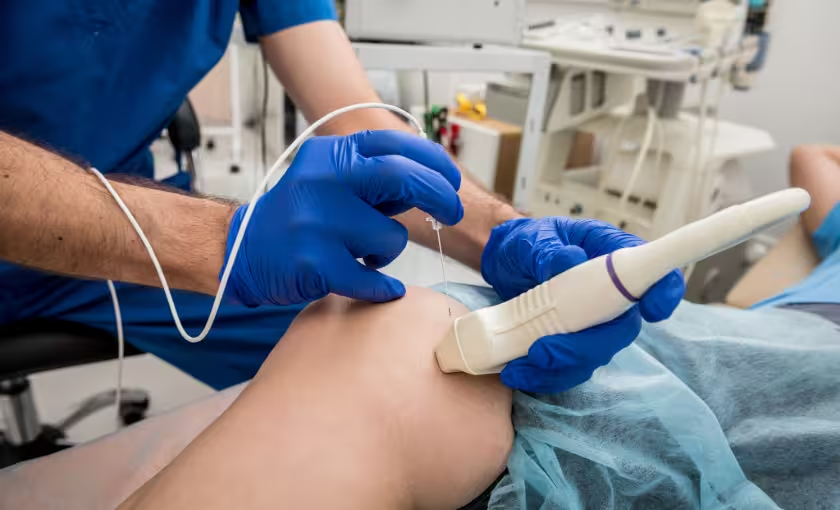
Diagnostic testing, typically including duplex ultrasound examination, provides detailed information about vein anatomy and function that is essential for accurate diagnosis and treatment planning. This non-invasive test can identify the source of venous reflux and guide appropriate treatment selection.
Treatment planning involves discussing the various treatment options available, their benefits and risks, and developing a plan that meets the patient's goals and preferences. This planning process should include discussion of expected outcomes, recovery time, and long-term management strategies.
Patient education is a crucial component of professional evaluation, ensuring that patients understand their condition, treatment options, and what they can do to optimize their outcomes and prevent future problems. Well-informed patients are more likely to achieve successful outcomes and maintain their results over time.
Living with Varicose Veins: Management Strategies
For patients who are not ready for treatment or who want to optimize their outcomes before and after treatment, understanding management strategies can help minimize symptoms and prevent the progression of varicose veins.
Daily management techniques include leg elevation, regular movement, and wearing appropriate compression garments when recommended. These simple measures can help reduce symptoms and may slow the progression of varicose veins.
Exercise recommendations focus on activities that promote healthy circulation, particularly those that engage the calf muscles and avoid prolonged static positions. Walking, swimming, and cycling are excellent choices for individuals with varicose veins.
Lifestyle modifications that support vein health include maintaining a healthy weight, staying hydrated, eating a balanced diet, and avoiding prolonged periods of standing or sitting. These modifications can help reduce symptoms and support overall vascular health.
Symptom management strategies may include over-the-counter pain relievers, topical treatments for itching or discomfort, and techniques for managing swelling, such as leg elevation and compression. Understanding these strategies helps patients maintain comfort while considering treatment options.
Monitoring for changes in symptoms or appearance helps patients recognize when their condition may be progressing and when additional medical evaluation may be warranted. Regular self-assessment can help identify problems early when they may be easier to treat.
The Psychological Impact of Varicose Veins
Varicose veins can have significant psychological and social impacts that extend beyond their physical symptoms, affecting self-confidence, clothing choices, and participation in activities. Understanding these impacts helps validate patients' concerns and emphasizes the importance of addressing varicose veins comprehensively.
Self-image concerns related to the appearance of varicose veins can significantly impact quality of life, leading to avoidance of activities that expose the legs, such as swimming, wearing shorts or skirts, or participating in sports. These concerns are valid and can be effectively addressed through appropriate treatment.
Social limitations may develop as individuals with varicose veins avoid activities or situations where their legs might be visible, potentially leading to reduced participation in social, recreational, or professional activities. Treatment can help restore confidence and eliminate these limitations.
Clothing restrictions often develop as people with varicose veins choose clothing that conceals their legs, potentially limiting their wardrobe choices and affecting their personal style. Successful treatment can restore the freedom to wear any clothing with confidence.
Activity limitations may occur when varicose vein symptoms interfere with exercise, work, or recreational activities, potentially leading to reduced fitness, career limitations, or decreased enjoyment of life. Treatment can help restore full participation in desired activities.
Relationship impacts can occur when varicose veins affect intimacy or self-confidence in personal relationships. Open communication about concerns and appropriate treatment can help address these issues and restore confidence.
Conclusion: Empowering Informed Decisions About Vein Health
Understanding varicose veins empowers individuals to make informed decisions about their vein health, recognize when professional evaluation is warranted, and take proactive steps to prevent or address these common but treatable conditions. Knowledge about varicose veins helps dispel myths and misconceptions while providing the foundation for effective communication with healthcare providers.
The key to successful varicose vein management lies in understanding that these conditions are not simply cosmetic concerns but rather manifestations of underlying venous disease that can progress over time if left untreated. Early recognition and appropriate intervention can prevent complications while providing significant improvement in both appearance and quality of life.
Modern treatment options for varicose veins offer excellent outcomes with minimal discomfort and downtime, making it easier than ever for patients to address their vein problems effectively. Understanding these options helps patients feel confident about seeking treatment and achieving the results they desire.
BASS Vein Center's commitment to patient education and comprehensive vein care ensures that individuals have access to the information and expertise needed to make informed decisions about their vein health. The center's experience with thousands of patients provides valuable insights into what works best for different types of varicose vein problems.
For individuals dealing with varicose veins, understanding the condition is the first step toward effective treatment and improved quality of life. Armed with knowledge about causes, symptoms, risk factors, and treatment options, patients can take control of their vein health and work with experienced specialists to achieve optimal outcomes.
Don't let varicose veins continue to impact your comfort, confidence, and quality of life when effective treatments are available to address both the symptoms and appearance of these common conditions. Contact BASS Vein Center today at (925) 489-1684 to schedule a comprehensive evaluation and learn more about how modern varicose vein treatments can help you achieve healthier, more comfortable, and better-looking legs. Your journey toward better vein health begins with understanding your condition and taking the first step toward professional care.
Take the First Step to Ending Annoying Varicose Vein Discomfort.






.svg)