3 Most Common Causes Behind a Venous Leg Ulcer
Venous leg ulcers are open sores that develop when blood does not flow properly through the veins of the lower legs. They can be painful, slow to heal, and prone to infection. Common symptoms include swelling, heaviness, itching, aching, scaly skin, and dark discoloration around the wound. Because a venous ulcer is an open wound, it is vulnerable to bacteria—making prompt medical care essential.
Symptoms of infection may include worsening pain, increased redness, green or yellow drainage, fever, and a foul odor. If you notice these signs, seek medical attention immediately.
Below are the three most common causes behind venous leg ulcers and how each contributes to this serious condition.
1. Venous Disease (Chronic Venous Insufficiency)
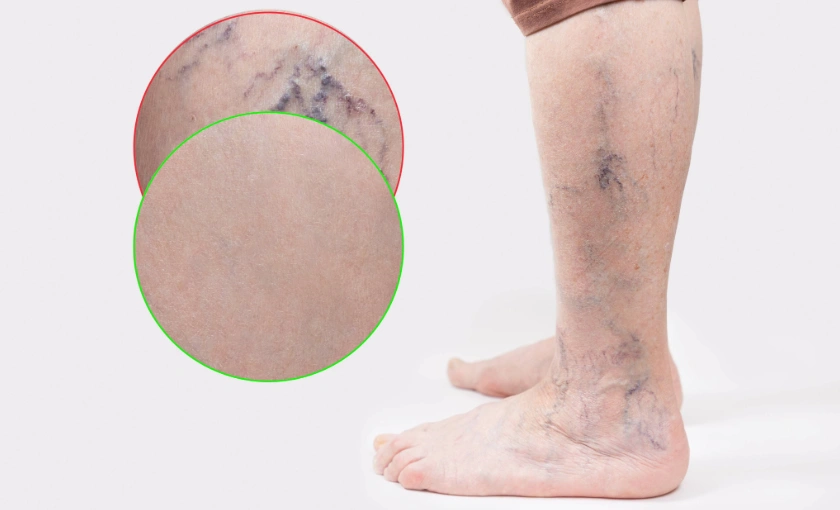
The leading cause of venous leg ulcers is chronic venous insufficiency (CVI)—a condition where the valves inside the leg veins no longer function properly. Healthy valves push blood upward toward the heart. When they weaken or fail, blood flows backward and pools in the lower legs, increasing vein pressure.
CVI may also cause:
- Spider veins
- Varicose veins
- Swelling (edema)
- Skin discoloration or thickening
- Inflammation
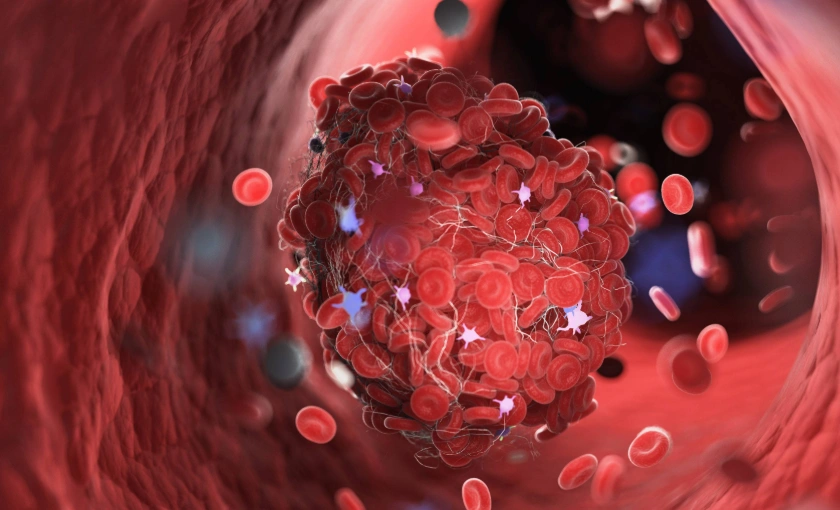
Venous insufficiency also increases the risk of thrombophlebitis (inflammation with clot formation) and deep vein thrombosis (DVT). DVT is more dangerous, as a clot can travel to the lungs and cause a life-threatening pulmonary embolism. Untreated venous disease eventually weakens the surrounding skin, leading to venous ulcers.
2. Leg Injury or Previous Surgery
Past injuries or surgeries—especially those involving the legs, hips, or ankles—can disrupt normal circulation and damage veins. Examples include:
- Fractures of the lower extremities
- Hip or knee replacement surgery
- Trauma leading to prolonged immobility
Reduced movement slows blood flow, increases venous pressure, and weakens the skin over time, making ulcer formation more likely.
3. Underlying Medical Conditions
Several health conditions can contribute to venous leg ulcers, either by affecting circulation or increasing swelling in the lower limbs. These include:
Lymphedema
Blockage of the lymphatic system causes fluid buildup, stretching the skin and making ulceration more likely.
Peripheral Arterial Disease (PAD)
Narrowed arteries restrict blood flow to the legs. While PAD is an arterial issue, poor circulation can delay healing and make venous ulcers more severe.
Diabetes
High glucose levels impair circulation and slow wound healing, increasing the risk of infection and chronic ulcers.
Obesity
Extra weight puts increased pressure on leg veins, worsening CVI and swelling.
Venous ulcers can heal with proper treatment, but recurrence is common if underlying conditions are not managed.
How to Prevent Venous Leg Ulcers
The most effective strategies include:
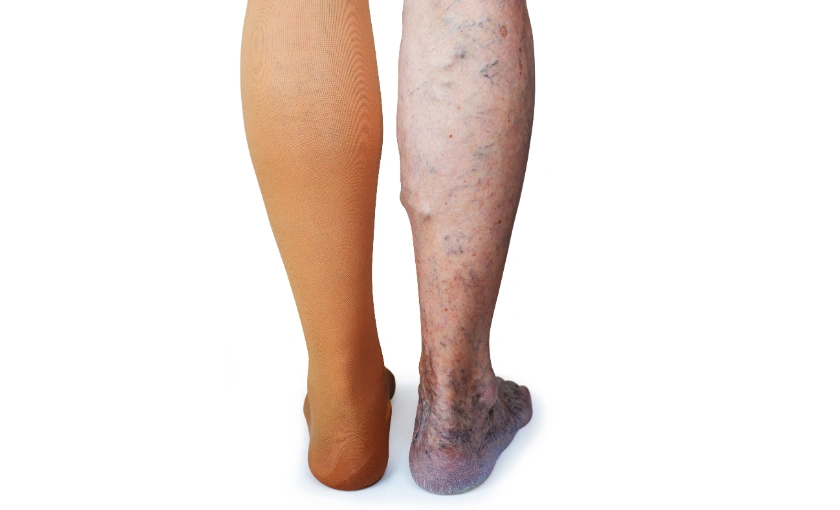
Compression Therapy
Compression stockings or sleeves help reduce swelling and improve blood flow. They should be worn during the day, especially during long periods of sitting or standing.
Regular Exercise
Walking is one of the best ways to improve circulation and prevent ulcers. Even short, frequent walks help strengthen the calf muscles, which act as a natural pump.
Leg Elevation
Elevate legs above heart level several times a day to reduce pressure and swelling.
Healthy Lifestyle Habits
Weight management, hydration, and a balanced diet all support vascular health.
Venous Ulcer Specialists at BASS Vein Center
BASS Vein Center offers comprehensive care for venous disease and chronic leg ulcers. Our team specializes in minimally invasive treatments such as:
- Conservative Vein Treatment
- Radiofrequency Ablation (RFA)
- VenaSeal™ Adhesive Closure
- Sclerotherapy
- Ambulatory Phlebectomy
With over 24,000 procedures performed, multiple East Bay locations, and a dedicated team of vascular surgeons, we provide expert care for varicose veins, spider veins, venous insufficiency, and chronic venous ulcers.
If you are experiencing symptoms or have a non-healing wound on your leg, schedule a consultation today. Early treatment improves healing and reduces the risk of future ulcers.
Frequently Asked Questions
1. What is the main cause of venous leg ulcers?
Most venous ulcers are caused by chronic venous insufficiency, where damaged vein valves lead to pooling blood and increased pressure.
2. How long does it take a venous ulcer to heal?
With proper treatment, most venous ulcers heal within 3–4 months. Severe cases or underlying conditions may slow healing.
3. Can venous ulcers be prevented?
Yes. Compression therapy, regular walking, weight management, and treating venous insufficiency can significantly reduce recurrence.
4. When should I seek medical care for a leg ulcer?
Any open wound on the leg—especially one that doesn’t heal—should be evaluated. Signs of infection require immediate medical attention.
References
- Wounds UK. Best Practice Statement: Holistic management of venousleg ulceration. https://www.livewellsouthwest.co.uk/wp-content/uploads/2025/05/Best-Practice-Statement-Management-of-Venous-leg-Uleceration-2nd-edition.pdf
- American Academy of Family Physicians. Venous Ulcers: Diagnosis and Treatment. https://www.aafp.org/pubs/afp/issues/2019/0901/p298.html
- NCBI Bookshelf. Venous Leg Ulcer. https://www.ncbi.nlm.nih.gov/books/NBK567802/
- Royal College of Surgeons. Comissioning Guide: Varicose Veins. https://www.rcseng.ac.uk/-/media/Files/RCS/Standards-and-research/Commissioning/Commissioning-guide-for-varicose-veins_Published.pdf
Note: Coverage varies between insurance plans. Please check with your insurance provider before scheduling. BASS Vein Center will verify your benefits so you understand any out-of-pocket costs ahead of treatment.
Medical Disclaimer: The information provided in this blog is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. BASS Medical Group does not endorse any specific tests, treatments, procedures, or opinions referenced in this content. Individual results may vary. Always consult with your physician or a qualified healthcare provider regarding any medical concerns or before making changes to your health regimen.