Does Insurance Cover Vein Treatment or Vein Surgery?

Does Insurance Cover Vein Treatment?
Often, yes—insurance may cover vein treatment when it is medically necessary, not purely cosmetic. Coverage depends on your plan, your symptoms, ultrasound findings, and whether you meet your insurer’s clinical criteria.
In general:
- Medically necessary vein treatment (for symptoms or complications) is more likely to be covered.
- Cosmetic treatment (appearance-only concerns with no symptoms) is more likely to be denied or not covered.
Because every plan is different, the most reliable step is a benefits verification and clinical evaluation.
What Makes Vein Treatment “Medically Necessary”?
Insurance companies typically consider vein treatment medically necessary when there is evidence of venous reflux or chronic venous insufficiency and it is causing symptoms or health risks.
Common medical-necessity reasons include:
- Leg aching, heaviness, throbbing, or fatigue
- Swelling (especially ankle/lower leg swelling)
- Skin changes near the ankle (discoloration, irritation, thickening)
- Recurrent inflammation of veins (phlebitis)
- Non-healing wounds or venous ulcers
- Bleeding from varicose veins
- Functional limitations (pain affecting work or daily life)
If symptoms are documented and supported by imaging, coverage is more likely.
Why Insurance Sometimes Denies Vein Treatment
Even when patients have visible varicose veins, insurance may deny coverage for several common reasons:
1) The Treatment Is Considered Cosmetic
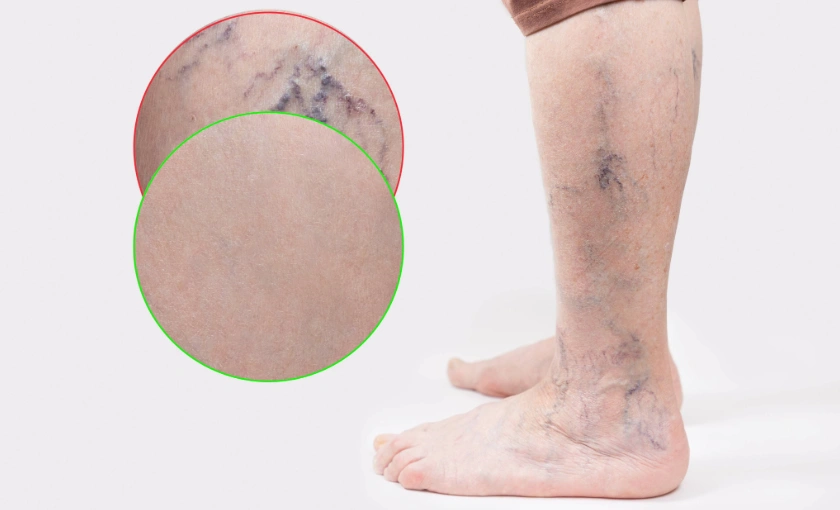
Spider veins and small surface veins are frequently categorized as cosmetic unless there is documentation of underlying venous disease.
2) No Ultrasound Evidence of Reflux
Most insurers require a venous duplex ultrasound showing reflux or venous insufficiency to justify treatment.
3) Conservative Therapy Was Not Tried First
Many plans require a trial of conservative care before approving procedures.
4) Symptoms Are Not Documented Clearly
Insurers often want symptom duration, severity, and impact on daily life in the medical record.
5) Prior Authorization Was Not Completed
Some treatments require pre-approval. Without it, claims can be denied even if the procedure would otherwise qualify.
Common Prerequisites for Full or Partial Coverage
While requirements vary by plan, these are typical steps insurers may require:
Venous Ultrasound
A diagnostic ultrasound documents reflux and maps which veins are involved.
Conservative Treatment Trial (Often Compression Stockings)
Many plans want proof of conservative therapy—often a compression stocking trial—for a defined period (commonly several weeks). Your provider documents whether symptoms improved or persisted.
Symptom Documentation
Insurers typically want notes showing:
- What symptoms you have (pain, swelling, heaviness, etc.)
- How long you’ve had them
- How they affect daily activities
- What you tried (compression, elevation, movement)
Prior Authorization
Your provider submits clinical notes and ultrasound findings to the insurance plan for approval before scheduling certain procedures.
Some plans may approve partial coverage (for certain veins or certain procedures) depending on findings.
Which Vein Treatments Are More Likely to Be Covered?
Coverage depends on medical necessity, but commonly covered treatments (when criteria are met) may include:
- Endovenous ablation (laser or radiofrequency) for refluxing veins
- Treatment for symptomatic varicose veins when ultrasound confirms venous insufficiency
- Ultrasound evaluation and follow-up as part of diagnosing vein disease
Treatments for spider veins only are more likely to be categorized as cosmetic, although some patients have spider veins plus underlying reflux—an evaluation helps clarify this.
What You Can Do to Improve the Chances of Approval
If you are trying to get vein treatment covered, these steps help:
- Get a clinical evaluation with symptom documentation
- Complete a venous duplex ultrasound (if indicated)
- Follow recommended conservative therapy (especially compression)
- Keep track of symptom patterns (worse at end of day, worse with standing, etc.)
- Ensure prior authorization is submitted before scheduling procedures that require it
At BASS Vein Center, our team helps guide patients through this process, including confirming benefits and submitting required clinical documentation.
How to Check If Your Plan Is In-Network With BASS Vein Center
Because network status and plan rules vary, the fastest way to reduce surprises is to confirm:
- Whether BASS Vein Center is in-network for your plan
- Whether your plan requires a referral
- Whether prior authorization is needed
- Expected deductible, copay, or coinsurance
We also maintain a page that we update regularly with insurance plans we accept. You can view it here: Insurances We Accept (BASS Vein Center). Please note that our standard coverage disclaimer still applies, and benefits can vary by plan and medical necessity.
To schedule a consultation or ask about coverage verification, call 925-477-3030.
Note: Coverage varies between insurance plans. Please check with your insurance provider before scheduling. BASS Vein Center will verify your benefits so you understand any out-of-pocket costs ahead of treatment.
Medical Disclaimer: The information provided in this blog is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. BASS Medical Group does not endorse any specific tests, treatments, procedures, or opinions referenced in this content. Individual results may vary. Always consult with your physician or a qualified healthcare provider regarding any medical concerns or before making changes to your health regimen.