How to Prevent Varicose Veins From Getting Worse

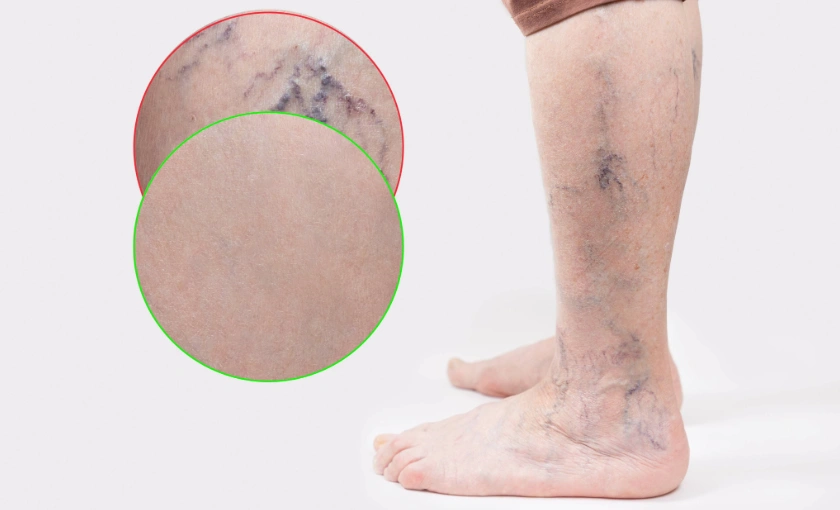
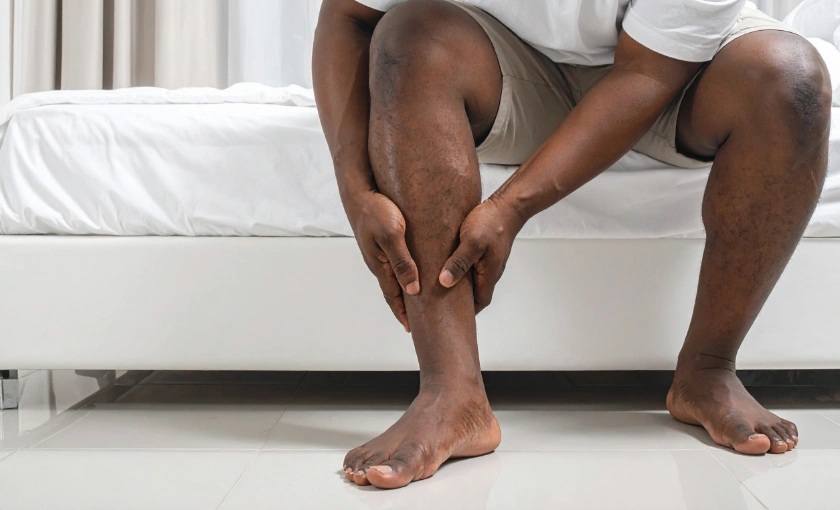
Varicose veins are enlarged, twisted veins caused by weakened or damaged vein valves. These valves normally keep blood flowing upward toward the heart. When they fail, blood pools in the lower legs, leading to swelling, heaviness, aching, and discomfort. While medical treatment may ultimately be needed, there are several effective steps you can take at home to prevent varicose veins from worsening.
Do I Need Varicose Vein Treatment?
If varicose veins are causing significant pain, interfering with daily movement, or worsening over time, it’s a good idea to schedule a consultation with a vein specialist. At BASS Vein Center, we offer non-invasive and minimally invasive treatments performed in-office — no hospital visit required.
Early evaluation can help prevent complications such as inflammation, skin changes, and venous ulcers.
Ways to Prevent Varicose Veins From Getting Worse
Whether you’re delaying treatment, preparing for a procedure, or looking for ways to improve circulation, these lifestyle changes can help slow the progression of varicose veins.
1. Exercise Regularly and Maintain a Healthy Weight
Movement activates your calf muscles — the natural “pump” that helps push blood upward. Activities like:
- Walking
- Cycling
- Leg raises
- Swimming
can improve circulation and reduce pressure in the veins. If you are overweight, even modest weight loss can significantly decrease stress on your lower extremities and improve symptoms.
2. Avoid Long Periods of Sitting or Standing
Stagnant positions are one of the biggest contributors to venous disease. If you sit all day, stand up and take a short walk every hour. If you stand for long periods, take sitting breaks whenever possible.
Small adjustments such as shifting weight, stretching, or flexing the ankles can meaningfully boost circulation.
3. Avoid Tight-Fitting Clothing
Tight jeans, leggings, shapewear, and garments that restrict the waist, thighs, or calves can limit blood flow and worsen vein pressure. Choose loose-fitting, breathable clothing to reduce strain on your veins.
4. Wear Compression Socks or Support Hose
Compression garments apply gentle pressure to your lower legs, helping veins move blood back toward the heart. They may reduce:
- Swelling
- Pain
- Heaviness
- Throbbing
Support hose offer lighter pressure, while medical-grade compression socks provide stronger, targeted support. A vein specialist can help determine the right level of compression for you.
5. Elevate Your Feet
Elevating your legs above heart level is one of the most effective ways to improve circulation. Just 10–15 minutes of leg elevation several times a day can reduce swelling and help prevent varicose veins from progressing.
Try elevating your legs:
- On a stool while sitting
- Using stacked pillows on the couch
- With a wall-assisted leg raise
Find Varicose Veins Treatment Near Me
Varicose veins can be uncomfortable, unsightly, and sometimes a sign of deeper venous insufficiency. The specialists at BASS Vein Center diagnose and treat all forms of vein disease to help you feel better and restore healthy circulation.
Call 925-477-3030 today to schedule your consultation.
Frequently Asked Questions
1. Can varicose veins go away on their own?
No. Varicose veins do not disappear without treatment, but lifestyle changes can help manage symptoms and slow progression.
2. Do compression socks really help varicose veins?
Yes. They improve circulation, reduce swelling, and help prevent vein pressure from worsening.
3. Can crossing your legs cause varicose veins?
Crossing your legs does not cause varicose veins, but prolonged sitting can worsen symptoms.
4. When should I see a vein specialist?
You should be evaluated if you experience ongoing leg pain, swelling, skin discoloration, or worsening visible veins.
References
Note: Coverage varies between insurance plans. Please check with your insurance provider before scheduling. BASS Vein Center will verify your benefits so you understand any out-of-pocket costs ahead of treatment.
Medical Disclaimer: The information provided in this blog is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. BASS Medical Group does not endorse any specific tests, treatments, procedures, or opinions referenced in this content. Individual results may vary. Always consult with your physician or a qualified healthcare provider regarding any medical concerns or before making changes to your health regimen.