5 Common Causes of Spider Veins—and What You Can Do About Them
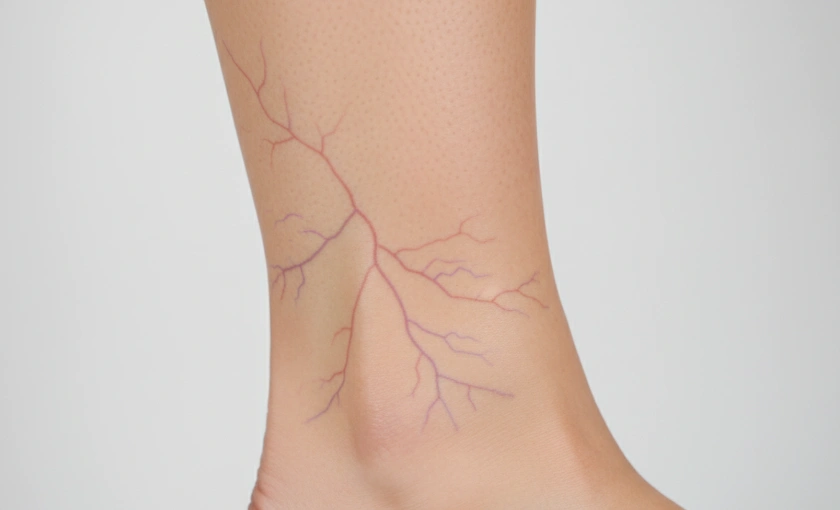
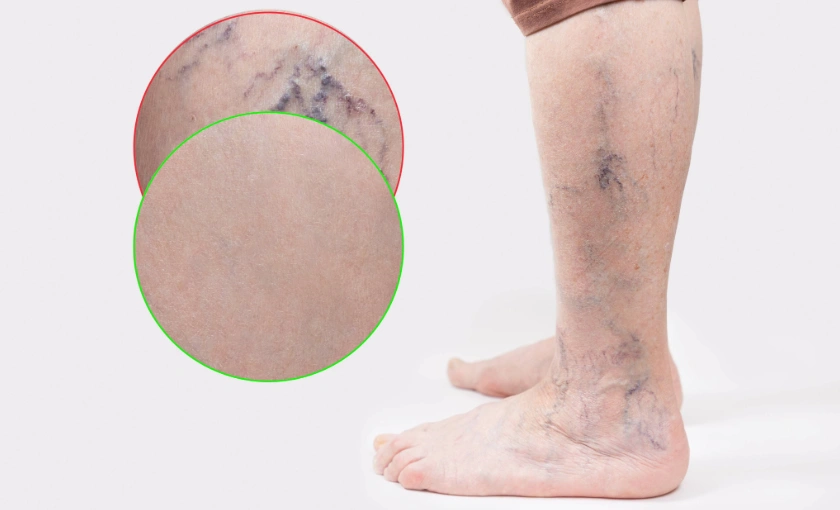
Spider veins are small, visible veins that develop close to the surface of the skin. They often appear red, blue, or purple and commonly form branch-like or web-like patterns. While spider veins are usually considered cosmetic, they can be an early sign of underlying venous insufficiency and may worsen over time without proper care.
Understanding what causes spider veins is the first step toward prevention and effective treatment.
What Causes Spider Veins?
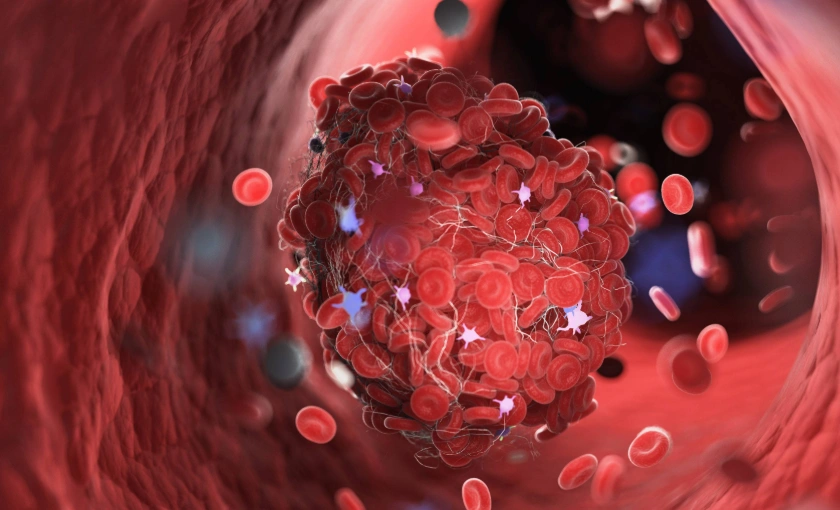
Spider veins develop when the tiny valves inside the veins weaken or fail. These valves are responsible for pushing blood back toward the heart. When they don’t function properly, blood pools in surface veins, causing them to stretch and become visible through the skin.
Although spider veins can affect anyone, they are more common in women and often linked to hormonal, genetic, and lifestyle factors.
1. Prolonged Sitting or Standing
Jobs or routines that require long periods of sitting or standing increase pressure in the leg veins. This pressure makes it harder for blood to circulate upward, contributing to valve failure and the formation of spider veins. Taking movement breaks, stretching, and walking regularly can help improve circulation.
2. Excess Weight or Obesity
Carrying excess body weight places additional strain on the circulatory system. Over time, this added pressure can weaken vein walls and valves, increasing the risk of spider veins and more advanced venous disease. Maintaining a healthy weight helps reduce stress on leg veins and supports overall vascular health.
3. Physical Inactivity
A sedentary lifestyle slows circulation and reduces the muscle contractions needed to push blood through the veins. Even low-impact activities such as walking, swimming, or cycling can significantly improve blood flow and reduce the likelihood of spider veins developing or worsening.
4. Genetics and Family History
Genetics play a major role in vein health. Studies suggest that up to 90% of people with spider veins have a family history of venous insufficiency. While genetics cannot be changed, lifestyle habits such as regular exercise, leg elevation, and compression therapy may help delay or minimize visible vein changes.
5. Pregnancy and Hormonal Changes
Pregnancy increases blood volume and places added pressure on leg veins. Hormonal changes also relax vein walls, making them more prone to stretching. Spider veins commonly appear during or after pregnancy and may fade over time, though some persist without treatment.
Treatment Options for Spider Veins
Lifestyle changes can help slow progression, but they typically do not eliminate existing spider veins. When spider veins become bothersome or continue to spread, professional treatment may be recommended.
Common treatments include sclerotherapy and other minimally invasive vein procedures designed to close damaged veins and redirect blood flow to healthier veins. These treatments are typically performed in-office with little to no downtime.
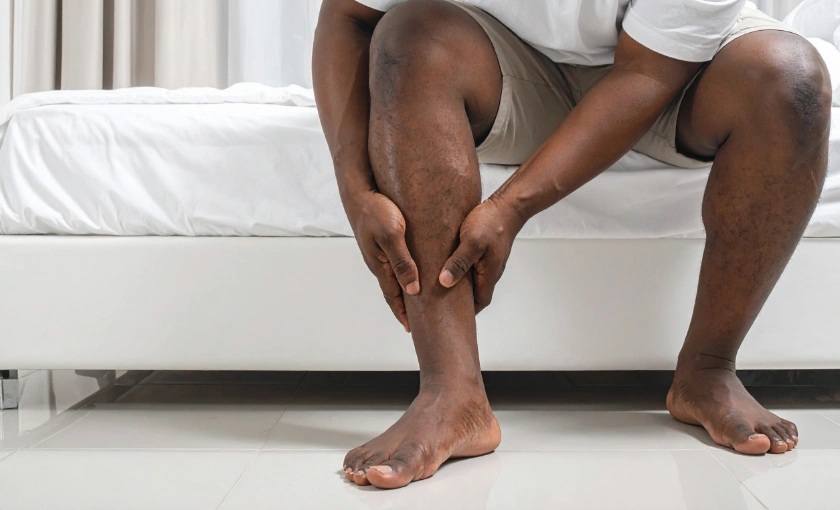
If spider veins are accompanied by leg pain, swelling, heaviness, or fatigue, a vein evaluation is important to rule out underlying venous insufficiency.
When to See a Vein Specialist
If spider veins are spreading, causing discomfort, or affecting your confidence, evaluation by a vein specialist can help determine whether treatment is appropriate. Early intervention may prevent progression into more serious vein conditions such as varicose veins.
At BASS Vein Center, patients receive comprehensive vein evaluations and personalized treatment plans using advanced, minimally invasive techniques.
Note: Coverage varies between insurance plans. Please check with your insurance provider before scheduling. BASS Vein Center will verify your benefits so you understand any out-of-pocket costs ahead of treatment.
Medical Disclaimer: The information provided in this blog is for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. BASS Medical Group does not endorse any specific tests, treatments, procedures, or opinions referenced in this content. Individual results may vary. Always consult with your physician or a qualified healthcare provider regarding any medical concerns or before making changes to your health regimen.